A continuous passive motion (CPM) machine can be used to move the knee joint. You will be able to walk with crutches or a walker. Knee immobilizers are used to stabilize the knee. A physical therapist will teach you specific exercises to strengthen your leg and restore knee movement. 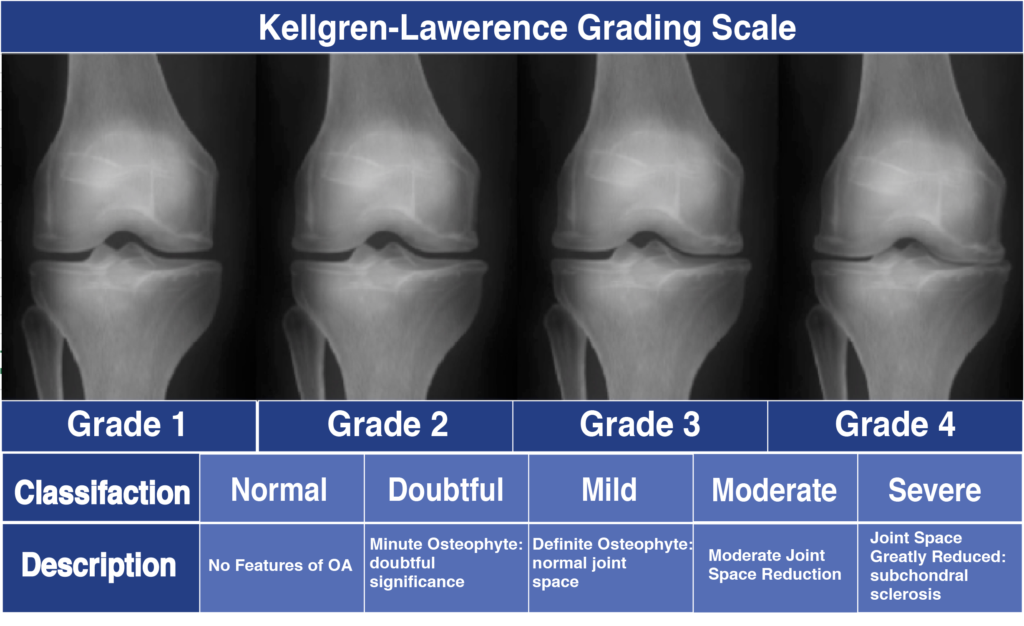
Rehabilitation begins immediately following the surgery. The incision is carefully closed, drains are inserted and a sterile dressing is placed over the incision. The entire joint is then irrigated and cleaned with a sterile solution. With all the new components in place, the knee joint is tested through its range of motion. To make sure the patella (knee cap) glides smoothly over the new artificial knee, its rear surface is also prepared to receive a plastic component. The femur and the tibia with the new components are then put together to form the new knee joint. 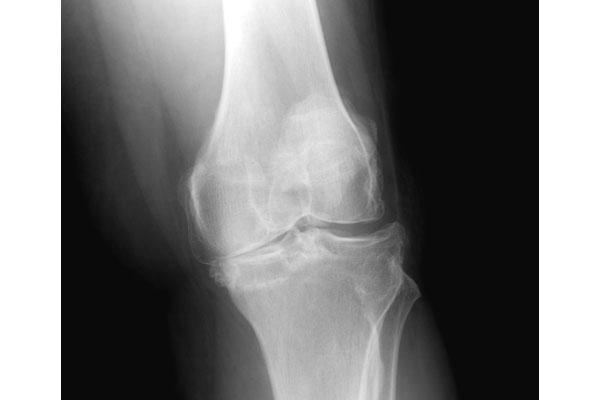
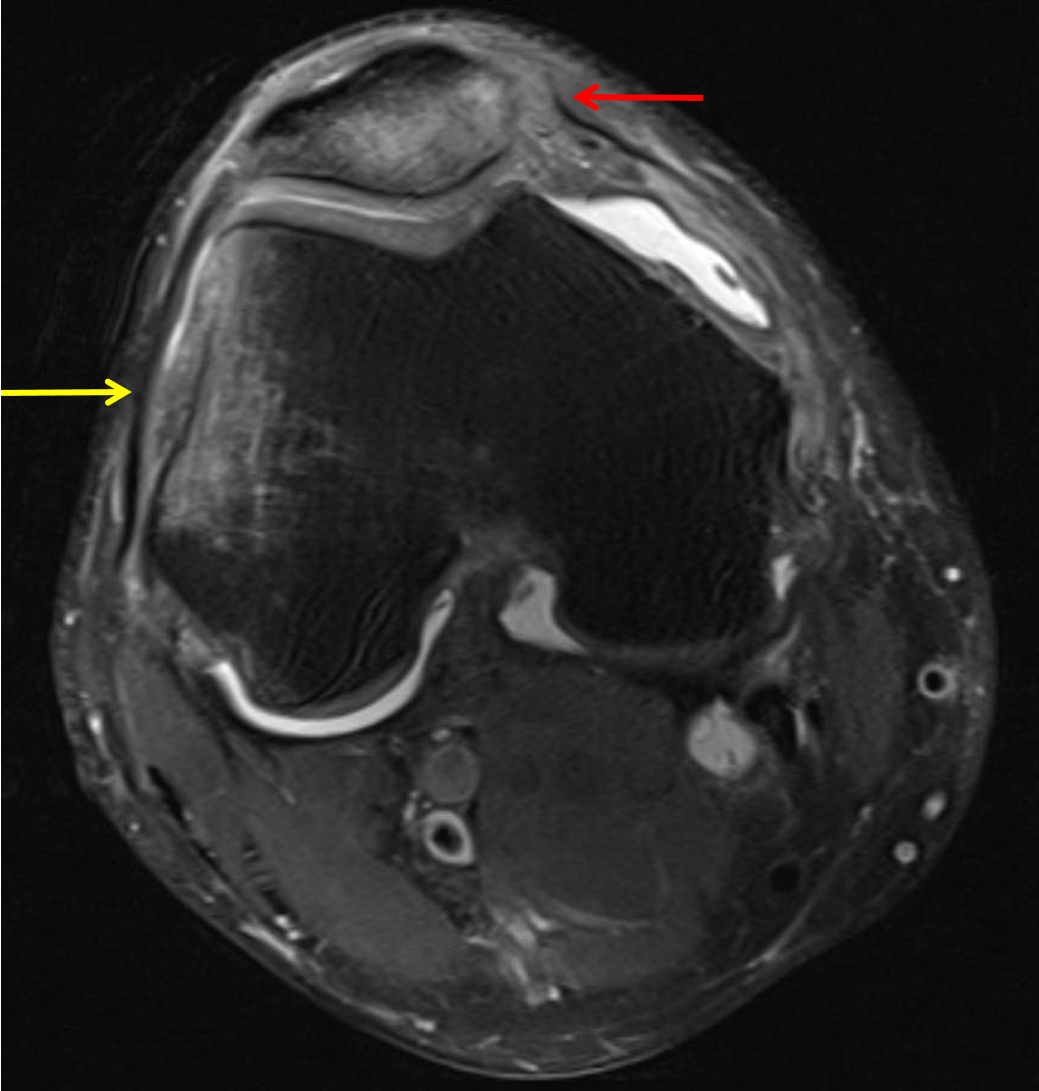
This plastic insert will support the body’s weight and allow the femur to move over the tibia, similar to the original meniscus cartilage. Your surgeon will place a plastic piece called an articular surface between the implants to provide a smooth gliding surface for movement. Next, the tibial component is secured to the end of the bone with bone cement or screws. This removes the deformed part of the bone and any bony growths, as well as creates a smooth surface on which the implants can be attached. The surgeon then cuts or shaves the damaged area of the tibia (shinbone) and the cartilage. The femoral component is attached to the end of the femur with or without bone cement. Then the damaged portions of the femur bone are cut at appropriate angles using specialized jigs. Your surgeon will make an incision in the skin over the affected knee to expose the knee joint. The surgery is performed under spinal or general anesthesia. Your doctor may recommend surgery if non-surgical treatment options have failed to relieve the symptoms. The goal of tricompartmental knee replacement surgery is to relieve pain and restore the alignment and function of your knee. Failure to obtain pain relief from medications, injections, physical therapy, or other conservative treatments.Chronic knee inflammation and swelling that is not relieved with rest or medications.Moderate to severe pain that occurs during rest or awakens you at night.Severe knee pain which limits your daily activities (such as walking, getting up from a chair or climbing stairs).Your doctor may advise tricompartmental knee replacement if you have: All of these factors can cause pain and restricted range of motion in the joint. In addition, the bones become thicker around the edges of the joint and may form bony “spurs”. In a normal joint, articular cartilage allows for smooth movement within the joint, whereas in an arthritic knee the cartilage itself becomes thinner or completely absent. Osteoarthritis is the most common form of knee arthritis in which the joint cartilage gradually wears away. Tricompartmental knee replacement surgery is commonly indicated for severe osteoarthritis of the knee. Lateral compartment – the area on the outside of the knee joint.Medial compartment – the compartment on the inside of the knee.Patellofemoral – the compartment behind the kneecap.The knee can be divided into three compartments: Arthritis (inflammation of the joints), injury, or other diseases of the joint can damage this protective layer of cartilage, causing extreme pain and difficulty in performing daily activities. The meniscus, the soft cartilage between the femur and tibia, serves as a cushion and helps absorb shock during motion. The knee is made up of the femur (thigh bone), the tibia (shin bone), and patella (kneecap). Tricompartmental knee replacement, also called total knee arthroplasty, is a surgical procedure in which the worn out or damaged surfaces of the knee joint are removed and replaced with artificial parts.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
